Definition
Hypoxia is a condition characterized by oxygen deficiency in the body tissues. Meanwhile, fetal hypoxia refers to oxygen deficiency in the fetal body tissues both before delivery, during pregnancy, and even after birth. The condition of hypoxia in newborns can be caused by a lack of oxygen condition that develops during pregnancy.
The formation, growth, and survival of the fetus in the womb depend on the mother's health and the normal development of the placenta. Continuous exposure to hypoxic conditions in the mother can lead to disruptions in placental development and cause negative effects on fetal growth.
The need for oxygen and nutrient intake increases as the placenta and fetus develop. Intrauterine hypoxia, or hypoxia that occurs in the womb, is a condition of oxygen deficiency that can originate from the mother, placenta, or fetus. This condition is typically identified through abnormal fetal heart rate patterns.
Causes
There are various conditions and diseases that can cause the fetus to not receive enough oxygen before, during, or after birth. Some of these conditions include:
Placenta
- Placental abruption, which is the separation of the placenta from its attachment site on the uterine wall. This condition is a pregnancy complication that causes bleeding in the third trimester and is associated with maternal and fetal death.
- Placental insufficiency is a condition where the placenta cannot provide enough oxygen and nutrients for the baby.
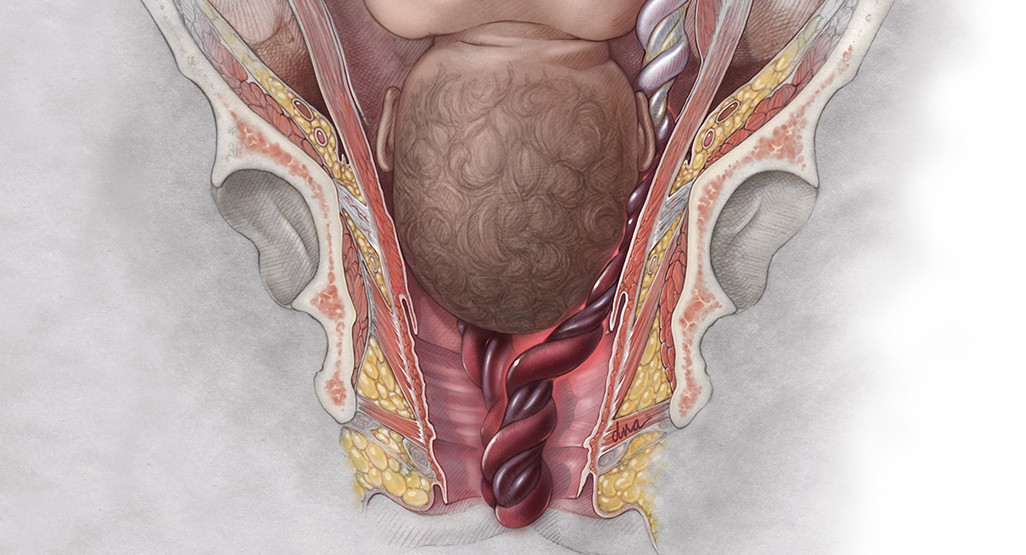
Umbilical cord
- Umbilical cord compression, which is pressure on the umbilical cord due to various reasons. Compression of the umbilical cord can inhibit the flow of oxygen and nutrients to the fetus, resulting in fetal oxygen deficiency.
- Umbilical cord knots, where the umbilical cord becomes knotted or twisted, hindering the flow of oxygen and nutrients to the fetus.
- Umbilical cord prolapse, when the position of the umbilical cord is ahead of the baby's head, between the baby's head and the cervix. This position is susceptible to umbilical cord compression.
Uterus
- Uterine rupture, which is the tearing of the uterine wall after 28 weeks of pregnancy, also occurs during childbirth.
Amniotic fluid
- Oligohydramnios, which is a low volume of amniotic fluid in the womb. Because the amount of amniotic fluid protecting the fetus is low, this condition can increase the risk of umbilical cord compression and inhibit the flow of oxygen and nutrients to the fetus.
- Meconium aspiration syndrome, where the baby inhales amniotic fluid contaminated by meconium during childbirth. Meconium itself is the baby's first stool. This condition can block the baby's airways.
Risk Factor
Factors that can increase the risk of hypoxia or low oxygen levels in the fetus include:
- Pregnant women might have comorbidities that can complicate pregnancy, including:
- Anemia
- Obesity
- Diabetes
- Hypertension or high blood pressure
- Pulmonary hypertension in the pulmonary blood vessels
- Kidney or liver disorders
- Congenital heart disease causing cyanosis symptoms in the skin
- Maternal pregnancy conditions, such as:
- Post-term pregnancy, which is a pregnancy lasting beyond 42 weeks
- Maternal age above 35 years
- Pregnancy with twins or more
- Fetal malposition, congenital abnormalities, or infections
- Low maternal oxygen levels
- Mother has a history of stillbirth in previous pregnancies
- Mother lives in high-altitude areas
- Maternal smoking
Symptoms
When the fetus is oxygen deficient, it typically shows signs of difficulty breathing, which can be observed from an abnormal heart rate during examination, such as:
- Tachycardia or an increase in fetal heart rate faster than 160 beats per minute
- Bradycardia or a decrease in heart rate less than 120 beats per minute
Other common signs and symptoms of fetal or neonatal hypoxia include:
- Decreased fetal movements felt by the mother
- Decreased fetal or neonatal heart rate
- Baby appears lethargic and weak at birth
- Bluish or pale skin color
- Weak muscle tone
- Poor reflexes
- Weak cry or no cry at birth
- Difficulty breathing
- Seizures after birth
- Presence of meconium in the amniotic fluid
Diagnosis
The doctor will inquire about complaints, medical history, and maternal pregnancy history. After that, the doctor will also perform a physical examination on the mother. Typically, the doctor will perform the following diagnostic tests to determine the level of fetal oxygen sufficiency:
Doppler Ultrasound (USG)
Fetal heart rate (FHR) is measured using Doppler Ultrasound (USG). The rate and pattern of fetal heartbeats are displayed on the ultrasound screen to determine whether they are normal. FHR provides information about fetal oxygen sufficiency. Normal fetal heart rate ranges from 120 to 160 beats per minute. In fetal distress conditions, when the fetus experiences worsening due to lack of oxygen, FHR shows less than 120 beats per minute or more than 160 beats per minute.
Cardiotocography (CTG)
Cardiotocography examination is performed to determine the response of heart rate to fetal movements and maternal uterine contractions. This examination can assess fetal distress earlier than Doppler Ultrasound.
Fetal Biometrics
This examination involves measuring parts of the fetus's body using ultrasound. If the examination results show that the fetal size is smaller than it should be, one of the reasons may be fetal oxygen and nutrient deficiency.
Management
The initial management for an unhealthy fetus involves intrauterine resuscitation. Several steps of management can be taken, including:
- Oxygen and fluid therapy
- Changing the mother's position or lying on one side, preferably the left side
- Amnioinfusion, which involves injecting fluid into the amniotic cavity (the sac surrounding and protecting the fetus) in cases of umbilical cord compression to reduce compression
- Tocolysis, which is a medication to delay premature birth by temporarily stopping contractions
- Administration of hypertonic dextrose infusion, which is high-concentration sugar solution
If the baby is in fetal distress, delivery must be promptly conducted. The doctor will induce uterine contractions to expedite the delivery process. If unsuccessful, the doctor may assist the mother in delivery using forceps or a vacuum extractor if necessary. However, if there are complications during delivery or meconium is present in the amniotic fluid, an emergency cesarean section is necessary. The surgical procedure should ideally be performed within one hour of detecting fetal distress.
If fetal distress causes the baby to aspirate meconium, the doctor must immediately clear the baby's airway after birth. This can be done with the assistance of a suction device and by placing a breathing apparatus (ventilator) if needed. Untreated fetal distress can lead to fetal death.
Complications
Complications of fetal hypoxia may include:
- Fetal growth abnormalities
- Fetal brain disorders
- Cerebral palsy, a congenital disorder involving brain impairment and muscle paralysis
- Jaundice in the baby
- Infections
- Premature birth
- Maternal vascular disorders in the placenta that can lead to preeclampsia
- Fetal death in utero
Prevention
Some cases of fetal hypoxia or fetal distress can actually be identified earlier. Therefore, it's important for pregnant women to undergo routine prenatal check-ups and always bring their pregnancy records to ensure proper monitoring.
When to See a Doctor?
If there are signs or symptoms as mentioned above, immediately consult a doctor for examination and appropriate management. It is to prevent worsening and complications for both the mother and the baby.
If you have risk factors as mentioned above, consult your doctor regularly to prevent your baby from experiencing fetal hypoxia or fetal distress.
- dr. Alvidiani Agustina Damanik
What are signs of fetal distress?. (2021). Retrieved 21 Februari 2022, from https://www.medicinenet.com/what_are_signs_of_fetal_distress/article.htm
Fetal distress. (2021). Retrieved 21 Februari 2022, from https://americanpregnancy.org/healthy-pregnancy/labor-and-birth/fetal-distress/#
Moldenhauer, J. (2021). Fetal Distress. Retrieved 21 February 2022, from https://www.msdmanuals.com/home/women-s-health-issues/complications-of-labor-and-delivery/fetal-distress
Fetal distress. (2020). Retrieved 21 February 2022, from https://www.pregnancybirthbaby.org.au/fetal-distress#