Definition
Orbital pseudotumor refers to the swelling of the tissue surrounding the eyeball within the orbital cavity, a bony cavity in the skull that houses the eyeball and its surrounding structures. These structures include eye muscles, blood vessels, eye nerves, tear glands, and fatty tissue. The orbital cavity's primary function is to protect the eyeball and other associated tissues.
The term "tumor" generally denotes "swelling or protrusion," while "pseudotumor" means "similar to a tumor." In orbital pseudotumor, the swelling results from inflammation rather than excessive cell growth as seen in tumors. This swelling is benign and does not metastasize to other tissues or body areas. However, if significant, the pseudotumor can exert pressure on other ocular structures and even extend beyond the orbit.
Inflammation in orbital pseudotumors can be localized or diffused. Localized inflammation typically affects eye muscles, tear glands, and the sclera (the white part of the eye), while diffuse inflammation usually involves the fatty tissue surrounding the eyeball. Orbital pseudotumor is a prevalent cause of painful orbital swelling, accounting for 8-11% of such cases, with the lacrimal gland being the most common site of inflammation.
The inflammation and swelling can be chronic or last for a long time, the bigger the swelling becomes, the surrounding structure can be pressed, including the eyeball. Orbital pseudotumor is a chronic condition that can affect one or both eyes, with a higher incidence of unilateral involvement in adults and bilateral involvement in children.
Causes
The exact cause of orbital pseudotumor remains unknown, but it is believed that infections and autoimmune conditions contribute to its development. Relevant infections include Streptococcus bacterial infections of the throat and viral infections of the upper respiratory tract. Several diseases are also associated with orbital pseudotumor, such as:
- Sarcoidosis (growth of inflamed cells)
- Tuberculosis
- Wegener's granulomatosis
- Giant cell arteritis
- Systemic lupus erythematosus (Lupus)
- Rheumatoid arthritis
- Polyarteritis nodosa
- Multifocal fibrosclerosis
- Crohn's disease
- Ulcerative colitis
Risk Factor
Orbital pseudotumor can occur at any age but is most commonly diagnosed in relatively young patients under 50 years old. It is more frequent in women and individuals with autoimmune diseases, where the immune system mistakenly attacks the body's own cells.
Recurrence risk factors include swelling of the optic nerve, non-responsiveness to steroid treatment, recurrence within three months, and abrupt discontinuation of steroid therapy.
Symptoms
Symptoms of orbital pseudotumor include:
- Severe eye pain, a hallmark symptom
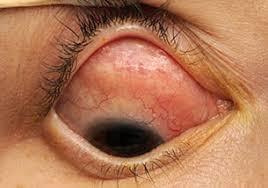
- Swelling and redness of the eyelids
- Visual impairment
- Limited eye movements if eye muscles are affected
- Double vision due to impaired eye movements
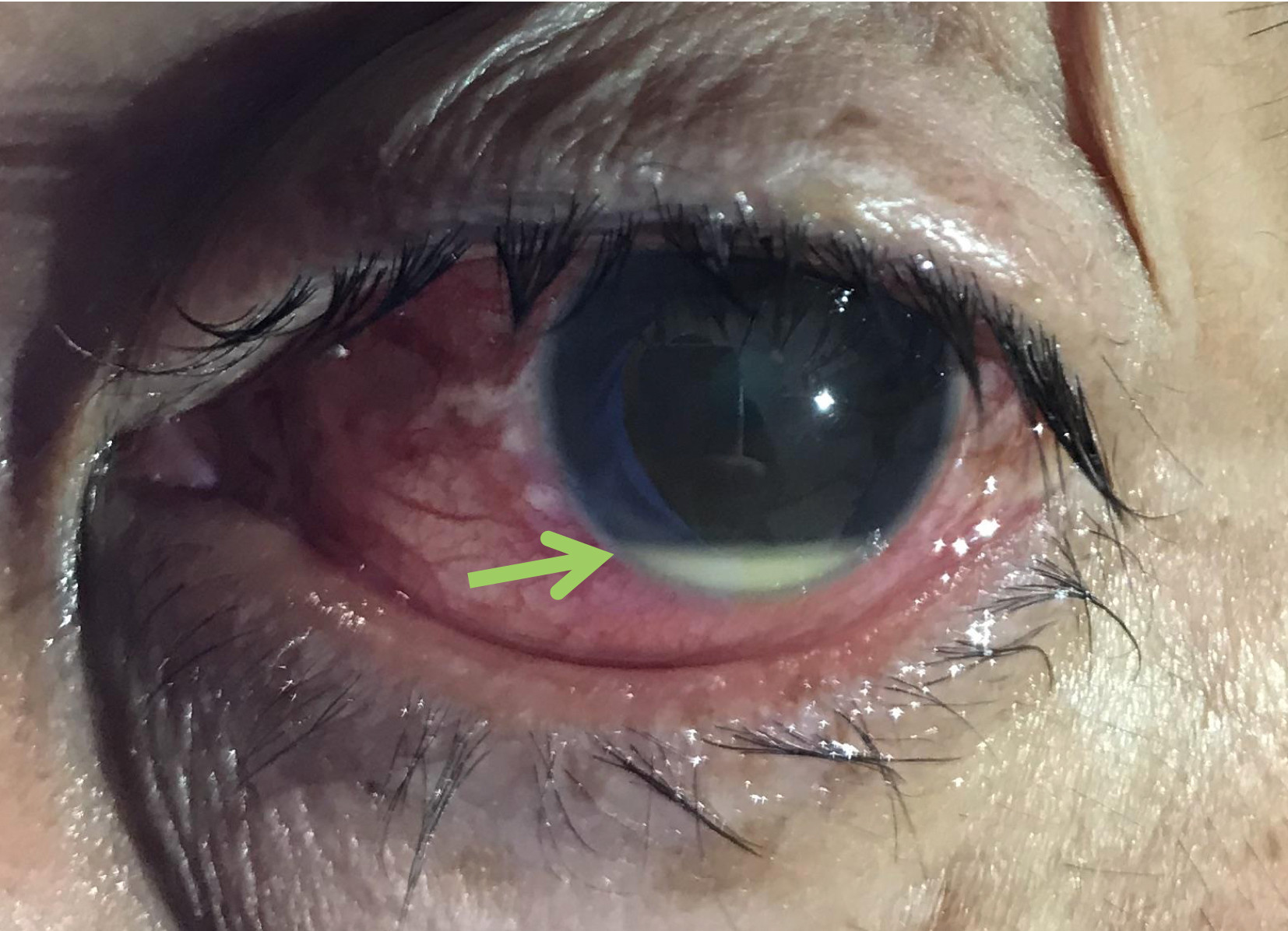
- Protrusion of the eyeball (proptosis) due to swelling and inflammation
- Eye redness (rare symptoms)
Diagnosis
If initial examination indicates signs of a pseudotumor, the patient can be referred to ophthalmologists. An ophthalmologist will conduct additional tests to find the cause and if they suspect of orbital pseudotumor, they will exclude other conditions causing orbital swelling, such as cancer or thyroid eye disease (Graves' ophthalmopathy).
Diagnostic tests may include brain CT scan, brain MRI, ultrasound of the eyes and head, x-ray of the skull, and biopsy, a procedure taking a sample of the suspected tumor tissues to be analyzed with a microscope.
Ultrasound or CT scan can help visualize inflammatory cells spreading in the orbital area, detect inflammation in the sclera or optic nerve swelling. The swelling of orbital pseudotumors generally do not have any clear borders.
Blood and spinal fluid examinations will show signs of inflammation. In classic cases of orbital pseudotumor, a rapid response to steroid medication can help confirm the diagnosis, often negating the need for a biopsy.
In atypical cases, a biopsy is necessary to check for infectious causes or specific diseases. An ophthalmologist may also conduct blood tests and X-rays to confirm related conditions such as sarcoidosis, tuberculosis, and Wegener's granulomatosis.
Management
Mild orbital pseudotumors may resolve without treatment. Severe cases typically respond well to corticosteroid treatment. If the swelling exerts significant pressure on the eyeball, surgery may be needed to remove part of the orbital bone to alleviate the pressure.
If surgical procedure is necessary, the Endoscopic Endonasal Approach (EEA) may be used. This minimally invasive technique that will not cause much body harm, accesses the orbit through the nasal cavity, minimizing tissue damage and promoting faster recovery.
Orbital pseudotumors are usually responsive to high-dose steroids. Unfortunately, inflammation often returns when steroids are stopped. The dosage should be tapered off slowly to prevent recurrence. In certain cases, low-dose chemotherapy and radiation may be required to control inflammation.
Over 75% of patients show improvement within 24-48 hours after starting steroid treatment. However, the reported cure rate is 37%, and the recurrence rate is about 52%, even with steroid treatment.
Complications
Severe cases of orbital pseudotumor can push the eyeball forward so that the eyelid cannot cover and protect the cornea (the outermost layer of the eye). This causes the eyes to become dry. The cornea or lining of the eye can become cloudy, inflamed, and develop into an ulcer or wound. In addition, the movement of the eye muscles can be disturbed so that they cannot direct the eyes properly and cause double vision.
Severe visual impairment can become permanent if orbital pseudotumor is left untreated or does not respond to treatment. Inflammation can spread to structures adjacent to the orbit such as the optic nerve and the intracranial or cranial cavity. Pseudotumor can exert pressure on some nerves in the brain and cause paralysis. Severe inflammation can also cause increased intraorbital pressure or glaucoma.
Prevention
Prompt and appropriate diagnosis and treatment, particularly with steroid drugs, can prevent eye function disorders and long-term vision loss.
When to See a Doctor?
Consult an ophthalmologist if you experience symptoms of orbital pseudotumor such as red eyes, eye pain, or visual disturbances. Early and accurate diagnosis and treatment can prevent symptom worsening and complications.
Looking for more information about other diseases? Click here!
- dr Hanifa Rahma
Orbital pseudotumor. (2020). Retrieved 8 April 2022, from https://medlineplus.gov/ency/article/001623.htm
Ronquillo Y, Patel BC. (2021). Nonspecific orbital inflammation. Retrieved 8 April 2022, from https://www.ncbi.nlm.nih.gov/books/NBK551576/
Orbital inflammatory pseudotumor. (2022). Retrieved 8 April 2022, from https://www.upmc.com/services/neurosurgery/brain/conditions/brain-tumors/orbital-inflammatory-pseudotumor#overview
Al-Zubidi N. (2022). Nonspecific orbital inflammation (idiopathic orbital inflammation, orbital inflammatory syndrome, orbital pseudotumor). Retrieved 8 April 2022, from https://eyewiki.aao.org/Nonspecific_Orbital_Inflammation_(Idiopathic_Orbital_Inflammation,_Orbital_Inflammatory_Syndrome,_Orbital_Pseudotumor)
Finger PT. Orbital pseudotumor. Retrieved 8 April 2022, from https://eyecancer.com/eye-cancer/conditions/orbital-tumors/orbital-pseudotumor/