Definition
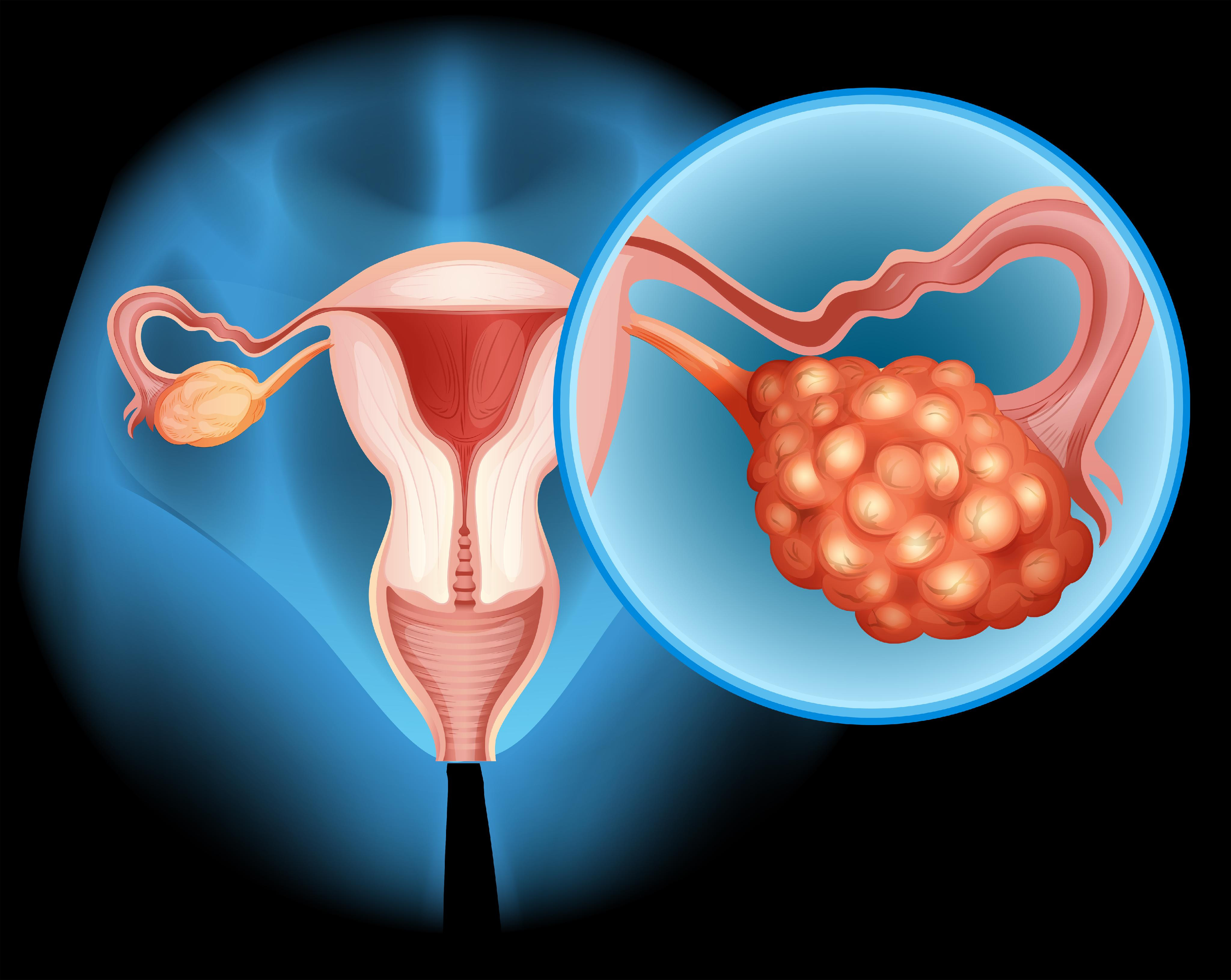
Ovarian carcinoma is a malignancy of the ovaries. This condition is caused by the growth of cancer cells in one or both ovaries. The ovaries are part of the female reproductive system, located on either side of the uterus. They are almond-sized and produce eggs as well as the hormones estrogen and progesterone.
According to Global Cancer Incidence data, there were 14,896 cases of ovarian cancer in 2020, with 9,581 deaths. Additionally, ovarian cancer is the third most common cancer in women in Indonesia.
Causes
Ovarian cancer begins when the cells in or around the ovary undergo structural changes in their DNA (DNA mutations). DNA contains instructions that regulate cells. Changes in DNA cause cells to grow and multiply rapidly, forming a tumor made up of cancer cells.
Cancer cells also continue to live when healthy cells should die. They can invade surrounding tissues and detach from the initial tumor, spreading to other parts of the body (metastasis).
Risk Factor
Factors that can increase your risk of ovarian cancer include:
- Advanced age. The risk of ovarian cancer increases with age, most commonly found in older adults.
- Inherited genetic mutations. A small percentage of ovarian cancers are caused by genetic mutations passed down from parents.
- Family history of ovarian cancer. If you have close relatives who have been diagnosed with ovarian cancer, your risk is higher.
- Overweight or obesity. Being overweight or obese increases the risk of ovarian cancer.
- Postmenopausal hormone replacement therapy. One of the postmenopausal hormone therapies is the hormone estrogen.
- Endometriosis
- Age at first menstruation and menopause. Starting menstruation early or going through menopause later, or both, can increase the risk of ovarian cancer.
- No experience of pregnancy. If you have never been pregnant, your risk of developing ovarian cancer may be higher.
Symptoms
Signs and symptoms of ovarian cancer may include:
- Bloating or abdominal swelling
- Feeling full quickly when eating
- Unexplained weight loss
- Discomfort in the pelvic area
- Fatigue
- Back pain
- Changes in bowel habits, such as constipation
- Increased frequency of urination
Diagnosis
Tests and procedures used to diagnose ovarian cancer include:
- Pelvic examination: During a pelvic exam, the doctor will insert their fingers into your vagina while pressing on your abdomen to feel your pelvic organs. The doctor will also examine the external genitalia, such as the vagina and cervix.
- Imaging tests: Tests such as ultrasound or CT scans of the abdomen and pelvis can help determine the size, shape, and structure of your ovaries.
- Blood tests: Blood tests may include organ function tests to assess your overall health. The doctor may also recommend a blood test for tumor markers that indicate ovarian cancer. For example, the CA 125 tumor marker can detect a protein often found in ovarian cancer cells. This test cannot confirm if you have cancer but can provide clues for diagnosis and prognosis.
- Surgery: Sometimes, the doctor cannot confirm the diagnosis until you undergo surgery to remove the ovary and have it examined in a laboratory for signs of cancer.
- Genetic testing: The doctor may recommend testing a blood sample to check for genetic mutations that raise the risk of ovarian cancer in the blood sample. Knowing about inherited genetic changes in your DNA will help the doctor make decisions about your treatment plan. You can also share this information with family members, such as siblings and children, as they may be at risk for the same genetic changes.
After ovarian cancer is confirmed, the doctor will use information from the tests and procedures above to determine the stage of the cancer. Ovarian cancer stages range from 1 to 4. Lower stages indicate the cancer is still confined to the ovaries. By stage 4, the cancer has spread to distant parts of the body.
Management
Ovarian cancer treatment usually involves a combination of surgery and chemotherapy. Other therapies may be used in certain situations.
- Surgery to remove ovarian cancer may include:
- Removal of one ovary
- Removal of both ovaries
- Removal of both ovaries and the uterus
- Surgery for advanced-stage cancer: If your cancer is advanced, the doctor may recommend surgery to remove as much cancer as possible. Sometimes, chemotherapy is given before or after surgery in these cases.
- Chemotherapy: Chemotherapy uses drugs to kill rapidly growing cells, including cancer cells.
- Targeted therapy: Targeted drug therapy focuses on specific weaknesses in cancer cells. By attacking these weaknesses, targeted drug therapy can cause cancer cells to die.
- Hormone therapy: Hormone therapy uses drugs to block the effects of estrogen on ovarian cancer cells. Some ovarian cancer cells use estrogen to help them grow, so blocking estrogen can help control the cancer.
- Immunotherapy: Immunotherapy uses your immune system to fight cancer.
- Palliative care: Palliative care is specialized medical care that focuses on providing relief from pain and other symptoms caused by serious disease.
Complications
Ovarian cancer complications can result from the disease itself or side effects of treatment. Treatment-related complications include:
- Infection
- Vaginal bleeding
- Blood clots
- Bleeding in the abdomen or pelvis
- Swelling of the legs
- Bladder or bowel problems
- Infertility
- Early menopause
- Anemia (lack of red blood cells), leukopenia (lack of white blood cells), thrombocytopenia (lack of platelets)
- Kidney damage
- Nerve damage
- Hearing problems
- Skin problems
Meanwhile, common complications of ovarian cancer include:
- Fatigue
- Nausea, vomiting, constipation
- Swelling in the legs or pelvis
- Anemia
- Fluid buildup in the abdominal cavity
- Bowel or bladder obstruction
- Fluid buildup in the lung lining
- Nutritional problems
Prevention
There is no sure way to prevent ovarian cancer. However, there are ways to reduce your risk, such as:
- Taking birth control pills: Ask your doctor if birth control pills might benefit you. Taking birth control pills reduces the risk of ovarian cancer, but these medications also have side effects, so discuss the pros and cons with your doctor based on your situation.
- Discussing your risk factors with your doctor: If you have a family history of breast and ovarian cancer, inform your doctor. The doctor can assess its impact on your cancer risk. You may be referred to a genetic counselor who can help you determine if genetic testing would be beneficial. If you have genetic changes that increase your risk of ovarian cancer, you may be given the option of surgery to remove your ovaries to prevent cancer.
When to See a Doctor?
You should see a general practitioner if you experience pain or discomfort in your pelvic area. Moreover, if you have unexplained weight loss, along with bloating or discomfort and complaints related to your reproductive organs, you should consult an obstetrician-gynecologist.
Looking for more information about other diseases? Click here!
- dr Ayu Munawaroh, MKK
Kementerian Kesehatan RI. Mengenal Kanker Ovarium, The Silent Killer. Available from: https://yankes.kemkes.go.id/view_artikel/1043/mengenal-kanker-ovarium-the-silent-killer
Ovarian cancer - Symptoms and causes. (2022). Retrieved 17 October 2022, from https://www.mayoclinic.org/diseases-conditions/ovarian-cancer/symptoms-causes/syc-20375941
Complications of Ovarian Cancer: How It Affects Your Body. (2021). Retrieved 17 October 2022, from https://www.everydayhealth.com/ovarian-cancer/complications/
Ovarian cancer. (2022). Retrieved 17 October 2022, from https://www.nhs.uk/conditions/ovarian-cancer/